Published: February 2026
As the climate in Wakefield is changing, we have been seeing an increase in warmer weather and rising temperatures. On hotter days the body tries to cool down by sweating and increasing blood flow to the skin. This can make some health conditions worse that affect the heart, blood vessels and lungs. Hot weather can cause dehydration, heat rash, heat stroke and heat exhaustion all of which can make people ill on their own or make long term conditions worse [1], [2]. Hot weather can also affect mental health and wellbeing and increase the risk of harmful events such as accidents and violence. Long periods of hot weather can put pressure on the health service and delivery of care too. It can lead to overheating in hospital buildings affecting staff wellbeing, may lead to equipment failure and can impact on supply chains [3].

Certain populations can be more vulnerable to the effects of heat and may find it harder to respond [4], this can lead to inequalities. On this page we give the number of people in Wakefield who may fall into some of the more vulnerable groups. The impact of heat on health is affected by three main factors:
- Exposure to heat
- Vulnerability to heat
- Ability to adapt and respond to heat
In the future, temperatures in Wakefield are expected to rise. Scientific modelling can be used to predict how things may change in the future. The impacts will depend on how much the temperature increases and how well we adapt to reduce the risks. One of the main models used in the UK is called UK Climate Projections (UKCP18). It is used by the UK Government and many other organisations to help plan for future climate change [5].
Headlines
- The climate of Wakefield is changing with higher average temperatures and more hot summer days that can affect people’s health.
- High temperatures impact health in a number of ways increasing risk of dehydration, heat stroke and exhaustion and make some long term conditions worse.
- Health and social services are also impacted by the heat due to more emergency admissions, overheating buildings and infrastructure issues.
- Urban environments and certain housing types, like flats, are more likely to overheat. Wakefield city centre is one area that has more of these types of housing.
- Younger or older people or those living with existing conditions are some of the people who are more vulnerable, many people in Wakefield fall into one or more of these groups.
- There are ways nationally and locally we are adapting to reduce the impact of heat these include: monitoring and responding to heat alerts, improving housing and city centre design, supporting vulnerable populations and providing health education and advice.
Heatwaves and heat alerts
High temperatures or long periods of hot weather lead to increasing impacts on health and health services. When temperatures are predicted to rise national and local plans are put into action to help reduce risks. The Met Office has developed a heatwave definition so everyone knows when a heatwave is underway. A UK heatwave threshold is met when a location records a period of at least three days in a row with daily maximum temperatures at or above the heatwave temperature threshold. The threshold varies by UK county and for Wakefield, in West Yorkshire, it is 25°C [6].
The United Kingdom Health Standards Agency (UKHSA) and the Met Office have developed a regional heat and cold health alert system which is updated daily. There are different levels of heat health alerts depending on the severity and action required, these are [7]:
- Green – no alert
- Yellow – response
- Amber – enhanced response
- Red – emergency response
Current alerts can be accessed through an online dashboard or you can sign up to email alerts [8]. In 2025 there were five heat alerts in Yorkshire and the Humber, two were amber and three were yellow.

Every year the UKHSA publishes an Adverse Weather and Health Plan to give some guidance on actions that need to be taken in the event of extreme weather including heat to protect health [9]. Local responses by health and social care providers to heat alerts are driven partly by national action card checklists to make sure staff are carrying out risk assessments and providing extra support relating to heat [10].
Wider responses to alerts are partly co-ordinated by local resilience forums (LRFs). LRSs are multi-agency partnerships made up of representatives from local public services, including the emergency services, local authorities, the NHS, the Environment Agency and others. The LRFs aim to plan and prepare for localised incidents and catastrophic emergencies. They work to identify potential risks and produce emergency plans to either prevent or reduce the impact of any incident on their local communities. Wakefield District is part of the West Yorkshire LRF [11].
In preparation for, or during periods of hot weather advice is available to local residents from a number of sources including Wakefield Council. Wakefield Council provides resources and links to further support on the Be Safe This Summer web page to help people keep healthy in hot weather [12]. Other adaptations and responses to heat are mentioned in later sections.
Heat effects on health
Periods of hot weather have been found to lead to an increase in mortality especially amongst older people, even temperatures of 25°C and above can have an impact in the UK where we are less used to higher temperatures. The increase in deaths is seen overall across a number of different causes affected by the heat [5].
Hot weather and high temperatures can lead to increased heat related illness such as sunburn, heat rash, heat stroke, heat exhaustion and dehydration. It can also make existing conditions worse including cardiovascular disease, respiratory conditions, which are also impacted by changes in air quality due to heat, and kidney disease. Heat can also make mental health conditions worse and lead to higher numbers of accidents and injuries. Warmer nights can also lead to difficulties with sleeping which can affect overall wellbeing [3]. The image below from the UK Health Security Agency (UKHSA) gives an overview of some of the direct and indirect effects of hot weather (Source). The United Kingdom Health Security Agency (UKHSA) present a dashboard containing syndromic surveillance data (the process of collecting, analysing and interpreting health-related data to provide an early warning of health threats). This includes, amongst other indicators, calls, appointments and attendances for patients presenting with symptoms related to hot weather, including heat, heatstroke and sunburn. This is taken from remote health advice (NHS 111), GP in-hours and emergency department reporting from across England. Indicators for hot weather are reported from 1 June to 30 September [14]. This helps in tracking how many heat related episodes are taking place and how it is affecting healthcare demand.
Health services themselves can also be impacted by hot weather, possible impacts include [3]: NHS Trusts and other health service organisations have heatwave plans to identify actions to be taken in preparation for and in the event of heatwaves of different levels. These plans and actions help reduce the impact of heatwaves on patient health and hospital services. Overheating incidents are recorded across the NHS identifying where the daily maximum temperature in each occupied ward or clinical area exceeded 26˚C. National data showed a 53% rise in such incidents from 2016/17 to 2023/24, with a peak in 2022/23 likely reflecting the record 40-degree temperatures in July 2022 [17]. In the 2024/25 financial year no such incidents were recorded in Wakefield [18]. Adult social care and other services that work with vulnerable people also face challenges during hot weather whilst making sure those they care for are kept safe. Advice on how to support vulnerable people is provided by the Government [4]. Advice for healthcare staff themselves about working in hot weather is provided by organisations including the Royal College of Nursing [19]. A UKHSA commissioned study was carried out in 2022 to help understand how social care practitioners coped during the heatwave in the summer of that year [20]. The study found most care workers had a good understanding of who was most at risk from the heat. They found domiciliary care workers found it most difficult to monitor and support those they were caring for. This was due to only seeing them for short periods and struggling due to travelling in hot cars between appointments. They found that those they were caring for wanted to keep wearing warm clothing or kept the heating on due to routine or not feeling the heat. A more recent study in London found care home staff were more likely to report care homes being uncomfortably hot whereas residents were less likely to report the same thing. Both these findings suggest older people may be more at risk of overheating without realising [21]. A Joseph Rowntree report in 2016 measured temperatures across four care home residences across England and found that several were above the recommended heat thresholds during summer months [22]. Wider infrastructure disruption to logistics or travel due to rail or road damage due to heat may also impact health and care services. This may include the delivery of medicines and essential equipment or ambulance journeys by road [23]. Ambulance call outs are known to increase during periods of hot weather from syndromic surveillance data [24] and wider research [25].
Mortality from heat
In 2024 looking at the four periods when heat alerts were in place it was found that across England there were estimated to be 1,311 (95% confidence interval [CI]: 929 to 1,692) heat-associated deaths, the highest heat-associated mortality rates were seen in those aged 85 years and over (521 per million population), and those aged 75 to 84 years (111 per million population); there were 2,844 and 4,087 heat-associated years of life lost, respectively, in these age groups [13].
Significant heat-associated deaths were seen in 3 out of the 4 heat episodes of the summer, despite only yellow heat-health alerts (HHAs) being issued. Significant heat-associated mortality was seen in the North West, West Midlands, East of England, London, South East and South West. In Yorkshire and Humber, where Wakefield is located, there was a non-significant increase (38 additional deaths, 95% confidence interval: -85 to 160).
Projections from the Health Effects of Climate Change report also showed expected increases in heat mortality into the future:
Annual average estimates of temperature-related mortality rate for Yorkshire and the Humber per 100,000 population for all ages. Lowest and highest estimates are based on the lowest and highest climate model realisations (from the suite of 12 provided in UKCP18) [5].
Health impacts

Warmer weather may also lead to a change in patterns of infection and vector borne diseases, this is a complex picture as the changes will depend on the type of infection considered. Some types of infectious diseases are more common in areas with higher temperatures whereas others are less common at hotter times of the year. Patterns of vector borne diseases may change as higher temperatures can increase the number of insects like mosquitos in the UK that could carry the pathogens that cause illnesses like malaria, Dengue fever, West Nile Virus and Zika. Currently these pathogens are not found in the UK but are being carefully monitored [15,16].
Health services, social care and wider impact
Heat exposure
Across the district of Wakefield the average temperature can vary, urban areas in cities can be affected by a heat island effect where temperatures are higher due to reflected heat and fewer green spaces. Outdoor temperatures can vary in direct sun or shade. Indoor temperatures can vary with top floor flats, terraced houses and west facing properties likely to be hotter [3]. From the 2021 Census 10.9% of households in Wakefield District are flats, maisonettes or apartments, but this is much higher in Wakefield City Centre, where almost half of households live in these types of properties [26]. Overcrowding affects 2.4% of households, again with higher levels in the city centre [27]. An image of some of the factors and solutions for the heat island effect are shown below: Housing quality, ventilation and person characteristics also influence indoor temperatures. People who may not be able to open windows due to air pollution, noise or safety concerns will also be at higher risk due to lack of additional ventilation [28]. In the Wakefield Adult Health survey 9% of respondents felt unsafe in their area in the day time and this rose to 45% after dark with higher figures in some areas of the district [29]. Those living with mobility problems may be at higher risk of overheating due to difficulties in opening windows or closing curtains to create shade [28]. People who are experiencing homelessness will also be more at risk as they will not have access to cool or sheltered spaces to avoid the heat. In Wakefield in the rough sleepers snapshot in England carried out in Autumn 2024 there were 19 people sleeping rough in Wakefield (5.3 per 100,000 population) [30]. People who live in deprived areas may also be more affected by heat as they have less resources to adapt their homes and environments [5].
Those living or staying in communal buildings such as care homes, hospitals, temporary accommodation or hostels and prisons are also at higher risk of heat effects as they may have less control over their local environment. In Wakefield there 97 CQC registered care homes, 2 hospitals (plus Dewsbury in the same Trust), nearly 270 households in temporary accommodation, including 243 children [31], and 2 prisons.
There are also those who have higher exposure to heat either indoors or outdoors e.g. those who are working in a hot environment or carrying out intensive work e.g. construction workers [3]. Several industries in Wakefield could be impacted by hot working environments including construction, logistics, warehouse work, glass manufacture and even office work if there are high indoor temperatures. Risk assessments are used to monitor the impact of heat and any adjustments needed in the workplace to protect staff. It is difficult to estimate how many people in Wakefield would be affected by heat due to their occupation.Heat island effect, housing, deprivation and ability to cool homes
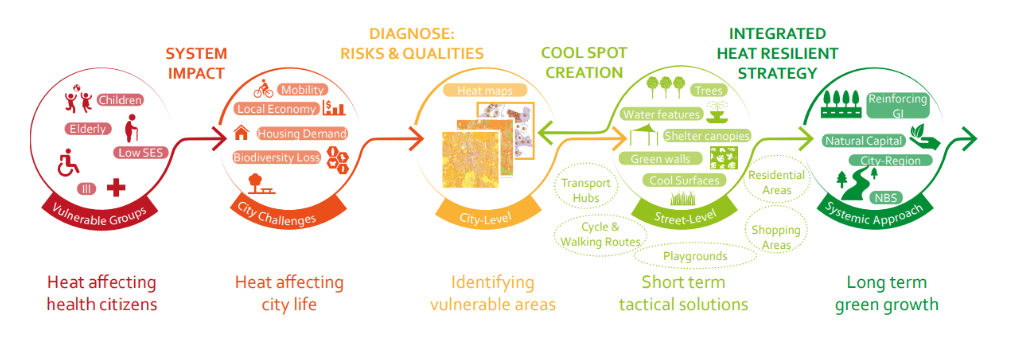
Adapted from: Spanjar, G., Bartlett, D., Schramkó, S., & Kluck, J. (2022). The Urban Heat Atlas: A standardised assessment for mapping heat vulnerabilities in Europe. Hogeschool van Amsterdam, Kenniscentrum Techniek. NBS – Nature Based Solutions, GI – Green infrastructure.
Staying in hospital or communal establishments
Working or being outdoors in hot weather
People who walk or cycle to work or who take part in physical activity outdoors may also be at higher risks from the effects of heat if they do not take precautions to reduce their exposure [3].
Vulnerable and at risk groups
Some groups are more vulnerable to heat, some of these are for: Examples of how health might impact heat response may include a physical disability which prevents someone being able to open windows or close curtains for shade or a mental health condition or learning disability which may make it difficult for someone to understand the risks of a heatwave or know what to do to respond.
The population of Wakefield District has been increasing, between the 2011 and 2021 Census the population of Wakefield increased by 8.4%, from around 325,800 in 2011 to 353,300 in 2021. This is higher than the overall increase for England (6.6%) and Yorkshire and the Humber (3.7%) [33]. Though Wakefield’s population rank remained the same being the 23rd largest local authority population in England. As of 2021, Wakefield is the sixth most densely populated of Yorkshire and The Humber’s 21 local authority areas, with around seven people living on each football pitch-sized area of land [33]. Older people are at higher risk due to a reduction in ability to control body temperature, mobility difficulties making it harder to keep hydrated or close curtains and open windows and having higher rates of health conditions which increase heat risk [3]. There are currently over 70,000 people in Wakefield District aged 65 and over. The population of Wakefield is expecting to have an aging profile over the next 25 years with the percentage of people aged 65+ increasing from 19.1% to 22% and the percentage of people aged 85+ increasing from 2.3% to 4.0% [34]. Children aged 0-5 can get hot more quickly and can’t always communicate they are too hot, which can lead to increased risks of heat stroke and dehydration. In Wakefield there are about 7,500 children in this age group [35]. Pregnancy can increase the risk of dehydration and heatstroke due to the extra demands and hormonal fluctuations. In severe cases high temperatures can lead to birth complications including low birthweight and preterm birth. In Wakefield in 2023 there were 3,502 live births in the District [36]. People with disability may find it difficult to respond to heat changes, in the 2021 Census 20.5% of Wakefield’s population (age-standardised) reported they had a disability, that is around 1 in 5 residents, 9.4% said that it limited their day to day activities a lot and 11.1% a little (age standardised percentages) [37]. In the latest primary care data 2,499 residents of all ages (0.7% of the Wakefield District population) have a learning disability [38]. Some medications can also reduce a person’s physiological ability to respond to heat including antipsychotics, antidepressants, diuretics and antihypertensive medication. The stability and efficacy of some medications can be affected by the heat as they need to be stored at optimal temperatures such as insulin and some types need to be stored out of sunlight [39]. Some people will fall into more than one risk group for the impact of heat on their health. They will then be affected by multiple factors; this means health advice needs to be individually tailored to ensure all factors are considered for each person. In some cases, those who are vulnerable to heat will also be vulnerable to other climate related risks such as cold weather, floods or droughts as there will be overlapping risk factors such as poor quality housing, deprivation and living with long term conditions and/or living with a disability [3].
Some areas of Wakefield are at higher risk both of exposure and vulnerability to the heat. A recent analysis by Friends of the Earth identified the areas in England most exposed to extreme heat. They used satellite-measured land surface temperature (LST) and modelled air temperature captured during the 2022 heatwaves [40]. Within these most exposed (high heat) neighbourhoods they also counted the number of care homes, nurseries and hospitals to identify areas at enhanced risk due to higher levels of vulnerable populations and infrastructure. These results were then aggregated to geographical areas called Middle Super Output Areas (MSOAs) which are defined by the Office for National Statistics. They comprise between 2,000 and 6,000 households and have a resident population between 5,000 and 15,000 persons. In Wakefield there are 45 MSOAs of which 19 were at high heat and enhanced risk and 26 were high heat but not enhanced risk. The areas at highest risk tended to be in Wakefield City, the Northeast and Southeast areas of the district. A separate analysis by Climate Just using a slightly different set of indicators to look at a wider section of the population who may be at risk found a similar pattern of areas [41].Overview
Some of the groups of people who are most likely to be more impacted are already facing disadvantages such as disability, deprivation or difficulties accessing services and additional heat effects may lead to greater inequalities [32]. Below is a summary of some at risk groups and an estimate of how many people of Wakefield are part of these groups, people can be in more than one group (those at risk due to housing are covered in the earlier section).
Groups at higher risk
The Wakefield population
Older people
Young children
During pregnancy
People with living with a disability, ill health and long term conditions
Some long terms conditions are directly impacted by increases in heat and the body’s response to it, others may be impacted by indirect effects such as the increase in air pollution increasing asthma symptoms during hotter weather. Heat can impact both physical and mental health. In the Wakefield Adult Health Survey in 2023 3 in 5 respondents reported having a long term health condition [29]. The number of people in Wakefield with some of the main conditions that can be affected by heat are below (people may have more than one condition, percentage of the population in brackets, data for 2024/25, taken from GP Quality Outcome Framework indicator figures in OHID Fingertips data):
Medications
Overlapping risks
Geographical areas of Wakefield at higher risk
Summary graphic of heat health risk groups in Wakefield
The summary below shows a summary of those groups at risk due to different exposures and some of the groups more vulnerable to heat effects:

Other factors impacted by heat
There are other areas that will be affected by hot weather but are not just impacted by heat these are not covered in this section but may be in future work and they include [33]:
- Drought
- Impacts on air quality and increased indoor and outdoor air pollution
- Loss of green spaces and biodiversity
- Higher levels of UV exposure from the sun increasing the risk of skin cancer and cataracts
- Food security – heat can affect crop harvests and yields, this can lead to the cost of food increasing and the availability of fruit and vegetables, more information on food poverty can be found on the related JSNA page
- National infrastructure impacts – the National Grid, computer networks and other major infrastructure such as water and sanitation systems could be impacted by prolonged periods of heat or very high temperatures
Adapting to heat effects
Each year there are usually several heat alerts and periods where temperatures rise. We can find ways to adapt to these heat periods and limit their impact on health as much as possible. National support and guidance is already available which is used locally [3]. The government are developing a Local Authority Risk and Adaptation Toolkit: Heat Edition which will help support local authorities to identify adaptations [42]. Adaptations to climate change including heat are part of the Third National Adaptation Programme (NAP3) [43] published by the UK Government and heat is covered in the Adverse Weather and Health Plan [44].
Adapting to heat effects can have lots of different approaches, many of these are already being used in Wakefield, these include:
- Adapting the built environment to reduce temperatures and increase ventilation
- Increasing access to shade, cool environments and drinking water across the district
- Raising awareness of the symptoms of heat exposure and sending out public health messages relating to heat
- Supporting organisations such as schools, care homes, charities and businesses to monitor and respond to heatwaves, including signposting to advice on how to assess and respond to the risk
- Planning for healthcare delivery during hot weather and making buildings such as hospitals, clinics and care homes resilient to heat effects
- Bringing together an adaptation plan for Wakefield District
Methods in construction and design of buildings such as adding shaded courtyard areas to blocks of flats, increasing the number of green and water features, making sure passive cooling and ventilation is part of the design process and using light covered surfaces can help make living environments cooler [45]. Adding shutters or additional shades to windows can also help reduce indoor temperatures. Giving advice to residents about approaches that can help such as closing curtains for shading, staying in cooler rooms and opening windows at night can also help. There is evidence from a national survey that some households are unprepared for overheating [46].
This can include increasing natural shade e.g. trees and opening public buildings as cool spaces e.g. libraries. Wakefield District has a woodland creation scheme as part of the White Rose Forest partnership with 25,000 trees planted in 2025. In February 2026 a further 10,000 free trees were given to residents, schools, farms, and community groups with help from the Woodland Trust. Provision of public cool spaces and the availability of water fountains are other ways we can support people in hot weather. London has a cool spaces map to show where cooler spaces can be accessed here and this is something that could be developed in Wakefield. Wakefield already has a Warm Welcome Spaces network.
Help and advice on staying cool and hydrated in warm weather is shared across the district by Wakefield Council, the NHS and other support agencies. Those health and social care professionals supporting people in their own homes can also help monitor temperatures and help with hydration [4]. There are a number of guidelines and advice for health professionals and unpaid carers. Several studies in England found some vulnerable and potentially vulnerable adults do not consider themselves at risk in hot weather and are not always aware of the effectiveness of important protective behaviours [47] so messages and advice are important.
Many local organisations and health services will have their own heatwave plans based on national guidance plus local intelligence, this includes for teachers and those working in early years settings [48]. Charities, voluntary sector organisations and businesses have access to advice through information and guidance relevant to their own needs such as the Health and Safety Executive for businesses [49]. Examples of changes could include: adapting working hours where possible, allowing water breaks and scheduling major events at cooler times of the day.
The NHS and local health services will have heatwave plans in place and these can be adapted and made futureproof to make sure delivery of services in Wakefield is not badly affected by spells of hot weather.
Across Wakefield resources, information and advice have been and continue to be developed to adapt to climate change including heat effects. Bringing together an adaptation plan which has health and equality as part of it’s focus will help streamline current and future efforts. This can help deliver on the District plan which sets out a vision of building a stronger Wakefield. One of the six ambitions is tackling climate change together.
References
1. UK Health Security Agency (2025) Beat the heat: staying safe in hot weather – GOV.UK
2.Xu J et al. (2025) Effects of extreme heat on physiology, morbidity, and mortality under climate change: mechanisms and clinical implications. BMJ 391:e084675
3. Mehrhof S, Bunn S (2024) Parliamentary Office of Science and Technology (POST) – Public health impacts of heat.
4. UK Health Security Agency (2024) Heat summary – supporting vulnerable people for all users.
5. UK Health Security Agency (2023) Health Effects of Climate Change (HECC) in the UK: Chapter 2. Temperature effects on mortality in a changing climate.
6. Met Office (2025) What is a heatwave?
7. UK Health Security Agency (2024) Heat-Health Alerting system.
8. UK Health Security Agency (2024) Weather health alert dashboard.
9. UK Health Security Agency (2025) Adverse weather and health plan.
10. UK Health Security Agency (2024) Heat Health alerting system.
11. Cabinet Office (2026) Local resilience forums: contact details.
12. Wakefield Council (2026) Be Safe This Summer.
13. UK Health Security Agency (2025) Heat mortality monitoring report, England: 2024.
14. UK Health Security Agency (2025) Summer seasonal environmental conditions.
15. UK Health Security Agency (2023) Health Effects of Climate Change (HECC) in the UK: Chapter 7: Effect of climate change infectious diseases in the UK.
16. UK Health Security Agency (2023) Health Effects of Climate Change (HECC) in the UK: Chapter 8: Direct and indirect effects of climate change on vectors and vector-borne diseases in the UK.
17. NHS England (2025) 4th Health and climate adaptation report NHS England.
18. NHS England (2025) Estates Returns Information Collection, Summary page and dataset for ERIC 2024/25.
19. Royal College of Nursing (2025) Working in hot weather
20. UK Health Security Agency (2024) Research exploring the experience of social care practitioners in relation to extreme temperatures.
21. Gupta R et al. (2021) Examining the magnitude and perception of summertime overheating in London care homes. Building Services Engineering Research & Technology. 42(6):653-675. doi:10.1177/01436244211013645
22. Gupta R et al. (2016) Care provision fit for a future climate.
23. Department for Transport (2025) Transport hazard summary series. Extreme heat
24. UK Health Security Agency (2026) National ambulance syndromic surveillance: weekly bulletins 2026
25. Xu Z et al (2023) Heat, heatwaves, and ambulance service use: a systematic review and meta-analysis of epidemiological evidence. Int J Biometeorol. 67(10):1523-1542.
26. 2021 Census (accessed 2026) 2021 Census interactive map of the percentage of people in Wakefield living in a flat, apartment or maisonette.
27. Wakefield JSNA (2025) Housing.
28. Yesudas MN (2024) UK Collaborative Centre for Housing Evidence – The heat is on: the growing problem of overheating in domestic homes in England and the need for a national strategy.
29. Wakefield JSNA (2023) Adult Population Health Survey.
30. Ministry of Housing, Communities and Local Government (2025) Rough sleeping snapshot in England: autumn 2024.
31. Ministry of Housing, Communities and Local Government (2026) Tables on homelessness
32. UK Health Security Agency (2023) Health Effects of Climate Change (HECC) in the UK: State of the evidence 2023.
33. Office for National Statistics (2025) How the population changed in Wakefield: Census 2021Understanding ageing in Wakefield.
35. LG Inform and Office for National Statistics (2025) Population, all persons aged 0 to 4 in Wakefield
36. Office of Health Improvement and Disparities (2026) Fingertips child and maternal health profile: pregnancy and birth
37. 2021 Census (accessed 2026) 2021 Census interactive map of the percentage of people with a long-term health problem or disability, including conditions or illnesses relating to old-age.
38. Office of Health Improvement and Disparities (2026) Fingertips learning disability profile.
39. Medicines and Healthcare products Regulatory Agency. Don’t let the heatwave affect your medicines: Three important tips from the MHRA
40. Friends of the Earth (2025) Which neighbourhoods are most vulnerable to heatwaves?
41. Climate Just (2025) Socio Spatial Heat Vulnerability Index, original reference: Lindley, S. J. et al. (2011) “Climate change, justice and vulnerability”, Joseph Rowntree Foundation Report, York.
42. UK Health Security Agency and Centre for Climate and Health Security (2026) Local Authority Risk and Adaptation Toolkit: Heat Edition.
43. Department for Environment, Food & Rural Affairs (2023) Third National Adaptation Programme (NAP3).
44. UK Health Security Agency (2025) Adverse Weather and Health Plan.
45.Lomas, KJ (2021) Summertime overheating in dwellings in temperate climates. Buildings and Cities, 2(1): 487–494.
46. Khosravi F et al. (2025) A nation unprepared: Extreme heat and the need for adaptation in the United Kingdom. Energy Research & Social Science. 124(104065).
47. Erens, B (2021) Public attitudes to, and behaviours taken during, hot weather by vulnerable groups: results from a national survey in England BMC Public Health, 21(1631).
48. UK Health Security Agency (2025) Looking after children and those in early years settings before and during hot weather: teachers and other educational professionals.
49. Health and Safety Executive (accessed 2026) Temperature in the workplace – 7. Heat Stress.
Resources
Wakefield Council Ready Set Summer heat advice page
Wakefield Council advice on some risks linked with activities that are more common during the summer and how the weather can have an impact on our health. Helping people plan ahead and prepare for a safe and healthy summer.
Heat – UK Government page bringing together useful resources
Heat presents a number of risks to health. UK Government information and guidance to help understand the risks of heat and consider actions to protect health.
NHS Heatwave advice page
NHS page – most of us welcome hot weather, but when it’s too hot, there are health risks. During heatwaves, more people than usual get seriously ill or die. If hot weather hits this summer, make sure it does not harm you or anyone you know.
UKHSA Heat warning alerts web page
The Weather health alerting system is provided by the UK Health Security Agency (UKHSA) in partnership with the Met Office. It’s intended to provide early warning to the health and social care sector, the responder community, the voluntary and community sector and government departments when adverse temperatures are likely to impact on the health and wellbeing of the population. The Weather health alerting system is made up of the Heat-Health Alerts (HHA) and Cold-Health Alerts (CHA). The Weather health alerting system underpins the Adverse Weather and Health Plan.
